Nightmare at home
Loading article...
Their home is no longer a sanctuary – it’s a prison of fear. At any moment, their mentally ill relative could strike and, for Sharon Burgess* and her elderly mother, that day could be fatal.
Burgess’ brother lives with them and, over the years, his violent outbursts have grown more frequent. Their house and yard has become his dumping ground. His rage-filled threats echo through the rooms, and police have been called multiple times to restore order.
The hardest part? Burgess’ 73-year-old mother, battling lupus, is the primary target. Her son sprays threats, death threats, and even roach spray at her during fits of rage.
His decline, Burgess says, began after his 2022 release from prison. Now in his 50s, he had been arrested in 2020 at Norman Manley International Airport while attempting to smuggle drugs overseas. Newly pregnant, his girlfriend had counted on him to secure a better life abroad. Instead, a two-year prison sentence — and an alleged sexual assault in custody — left him with deep mental and emotional scars.
The sexual assault claim was never formally reported.
“He was never like this before. My brother was a bright youth, a student at one of Jamaica’s top high schools,” Burgess said. “Now, we’re tired of calling the police. We don’t even have to tell them our address anymore.”
Cruel words
Last Friday, her mother recalled the cruel words her son often hurls at her: why she is still alive while others die, why no vehicle hits her to end her life, and why she survives while others succumb to diabetes and high blood pressure.
“Sometimes I don’t even recognise the person speaking,” the ailing woman said. Lupus may be attacking her organs but her son’s words pierce deeper than the disease ever could. Though he has not struck them physically, she said he has repeatedly sprayed roach killer on her as she sleeps.
“That’s his perception of his mother, who raised him without a father,” she said solemnly. “I feel sad but, because I am a child of God, I know the devil is using him to discourage me. Sometimes when I look into his face, I don’t even know that person.”
Outside, he stacks piles of debris and old appliances from the street, threatening anyone who touches them. The yard is chaotic. He has been admitted repeatedly to Bellevue Hospital for medication, only to return home and spiral again, they said.
For Burgess and her mother, fear and exhaustion are constant companions — trapped between caring for a loved one and protecting their own lives.
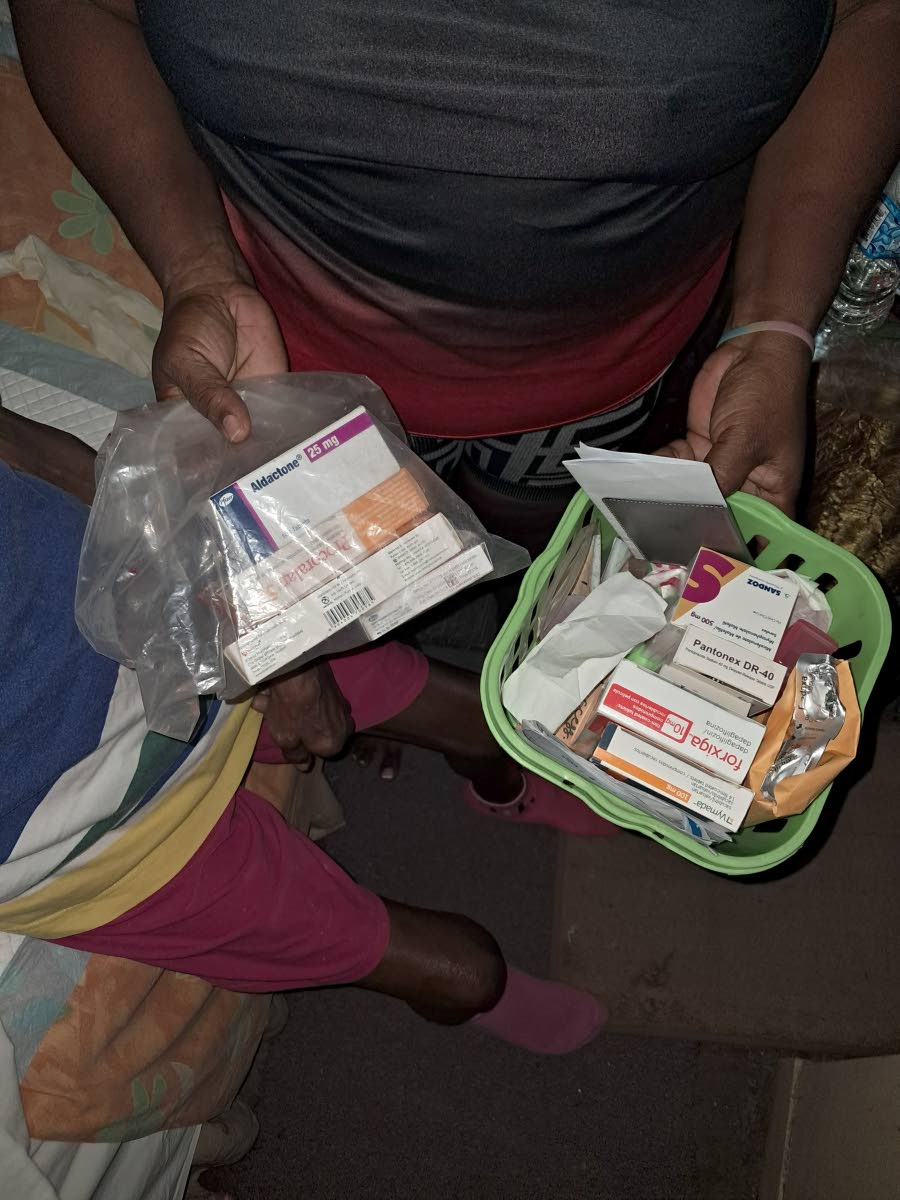
“I just want them to come for him. That way, I can live out the rest of my life in peace,” her mother said, displaying stacks of medication that have turned her into what she calls a “walking pharmacy”.
Burgess works as a caregiver herself, and managing her job, her mother, and her brother — whom she still loves despite his outbursts — is overwhelming.
However, the overwhelming experience of caring for a mentally ill relative is not unique to Burgess, according to Suzette Buchanan, CEO of Bellevue Hospital.
Some 400 patients have lived at Bellevue for decades without contact from relatives, in some cases not just because they were abandoned but because family members genuinely no longer believe they can handle the responsibility associated with looking after them.
Caring for these patients consumes a significant portion of the hospital’s $3.2-billion annual budget, covering food, clothing, and healthcare.
Buchanan said it is common for relatives to provide incorrect contact information, making follow-up impossible. Last week, she tried calling numbers for three social cases. None answered.
“We sometimes transport patients home by bus, only to find their relatives aren’t there. Many give false addresses. Some say they live downtown Kingston but they’re actually in Mandeville,” she said, noting that many long-term patients cannot recall their past addresses or relatives’ contact information.
Cannot provide a
long-term solution
Buchanan said Burgess’ experience is common in Jamaica, but the hospital cannot provide a long-term solution. Halfway homes and government-supported facilities are needed.
“Families have a responsibility to their relatives. If I keep him at Bellevue, he becomes a burden on our budget, which is unfair,” she said. “I understand caregiver burnout. I’m sympathetic. But there is a lifelong commitment, and [family] have to find a solution.
“I understand caregiver burnout, so I won’t approach it in a non-compassionate way. With caregiver burnout, these things do happen. But you have to understand that you have a lifelong commitment,” she charged.
The stakes are real. Last month, a woman was hacked to death, and her daughter was injured in Braeton, Portmore, St Catherine, by a man reportedly known to have a mental illness. Burgess’ brother has not harmed anyone in the community, though men once beat him after she asked them simply to talk to him.
“When I heard what they did, I nearly died,” she recalled.
Yesterday Dr Kevin Goulbourne, director of mental health and substance use at the Ministry of Health and Wellness, said emergency response teams are doing all they can, despite resource challenges. He noted that halfway homes for less volatile social cases are being considered, but funding remains limited.
In 2023, forensic psychiatric expert Dr Myo Kyaw Oo urged the Government to establish more halfway houses to accommodate cases like that of a 48-year-old schizophrenic who, after being admitted at the Kingston Public Hospital, was discharged into his 90-year-old mother’s care, despite her publicly expressing concern about the move.
The hospital had indicated that discharge of such patients only took place after a meticulous process.
“The Government of Jamaica doesn’t have halfway houses, supervised facilities for mentally ill,” Oo told The Gleaner at the time. “We should have some type of infirmaries ... halfway houses, supervised living facilities for discharged mentally ill who are crippled by the illness. But they are not to be treated as inpatient, they are to be treated as residents in those facilities.”
*Name changed
corey.robinson@gleanerjm.com